Insulin may be the most discussed, and most misunderstood, hormone in popular nutrition. It has been framed as the primary driver of fat storage, the reason carbohydrates are harmful, and the key to unlocking fat loss. Most of these claims are oversimplified. Understanding what insulin actually does, and how it works in balance with glucagon, provides a far more useful framework for thinking about metabolic health.
What Insulin Is and Where It Comes From
Insulin is a peptide hormone produced by beta cells in the pancreas. Its release is triggered primarily by rising blood glucose levels, typically after eating carbohydrates or protein. Insulin acts as a signaling molecule that tells cells throughout the body to take up glucose from the bloodstream, either for immediate use as fuel or for storage as glycogen (in muscle and liver) or fat.
Without insulin, glucose cannot effectively enter most cells. This is the physiological catastrophe at the center of type 1 diabetes; the immune system destroys the beta cells that produce insulin, leaving glucose unable to enter cells even as blood sugar climbs dangerously high.
What Glucagon Is and Why It Matters
Glucagon is insulin's functional counterpart, produced by alpha cells in the pancreas. Where insulin signals storage and uptake, glucagon signals release. It is secreted when blood glucose falls: during fasting, between meals, or during intense exercise.
Glucagon stimulates the liver to break down glycogen stores and release glucose into the bloodstream (glycogenolysis), and to produce new glucose from non-carbohydrate sources including amino acids and glycerol (gluconeogenesis). It also promotes fat breakdown (lipolysis) to supply free fatty acids as fuel.
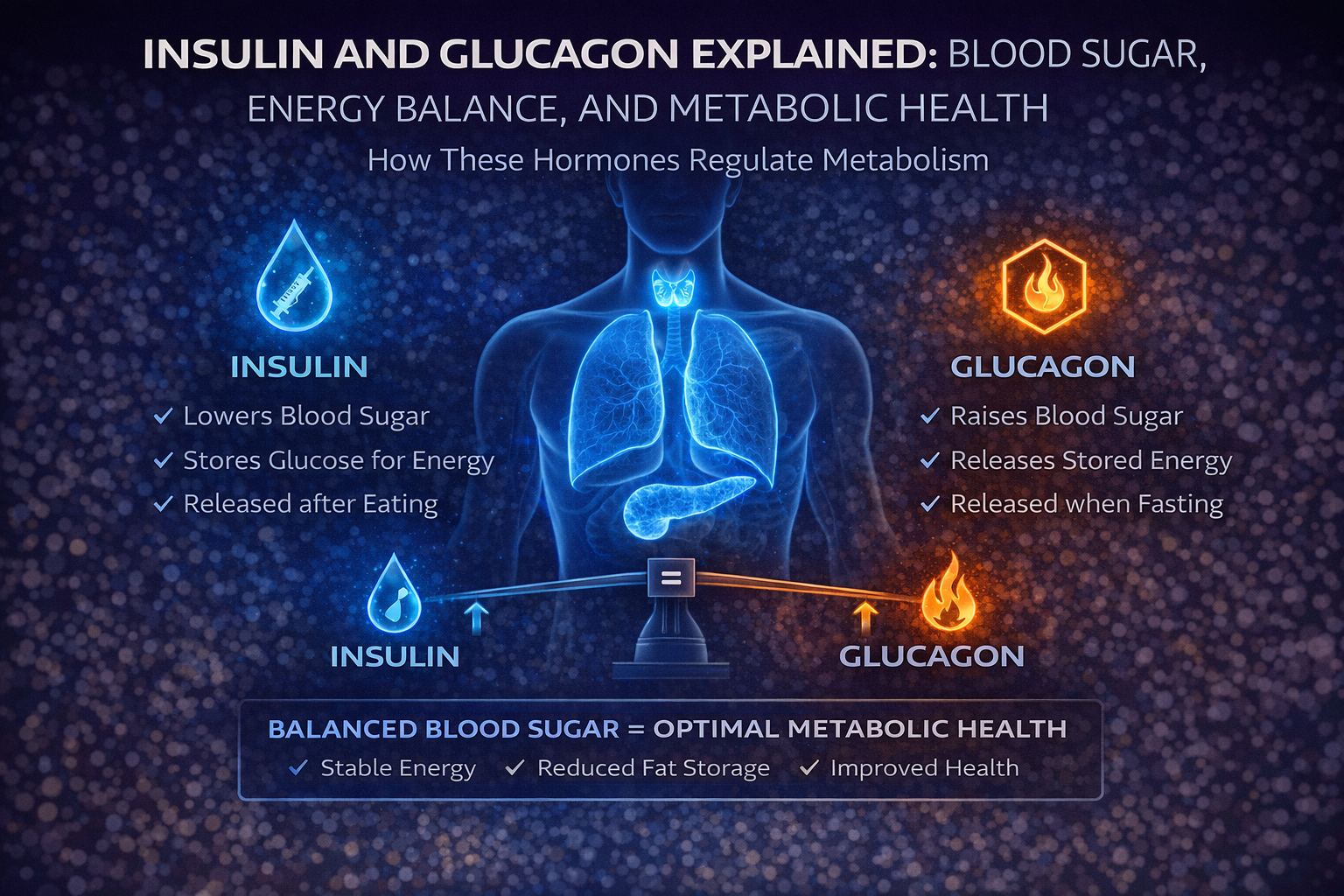
Insulin and glucagon operate in a continuous, dynamic balance. The fed state is characterized by elevated insulin and suppressed glucagon. The fasted state reverses this: glucagon rises, insulin falls, and stored energy is mobilized. Both hormones are normal. Both are necessary.
Insulin and Fat Storage
Insulin does promote fat storage; this is accurate. In a fed state, insulin facilitates the uptake of excess energy into adipose tissue. But it does not store fat in a vacuum. It stores fat in the context of a calorie surplus.
If total energy intake matches or is below expenditure, insulin-driven fat storage is offset by glucagon-driven fat mobilization during fasted periods. Net fat accumulation requires sustained surplus, not simply the presence of insulin. This distinction is why studies comparing isocaloric low-carb and high-carb diets consistently show similar fat loss outcomes when total calories and protein are matched.
Insulin is not your enemy. It is a nutrient-delivery hormone. The goal is not to suppress it permanently; it is to maintain a metabolic state where fat mobilization during fasted periods balances fat storage during fed periods. Calorie balance determines which side wins over time.
Insulin Resistance
Insulin resistance is a state in which cells become less responsive to insulin's signal. The pancreas compensates by producing more insulin, a state called hyperinsulinemia, to achieve the same blood glucose lowering effect. Over time, if the pancreas cannot keep pace with demand, blood glucose rises and type 2 diabetes develops.
Insulin resistance is driven primarily by excess body fat (particularly visceral fat), physical inactivity, and chronic calorie surplus, not by carbohydrate intake in isolation. It is reversible in most cases through weight loss, increased physical activity, and dietary improvements. Resistance training, in particular, meaningfully improves insulin sensitivity in skeletal muscle.
Improving Metabolic Health
The most effective lifestyle interventions for improving insulin sensitivity and glucagon balance are consistent: maintaining a healthy body composition, engaging in regular resistance training and aerobic activity, prioritizing sleep, managing chronic stress, and consuming a diet rich in fiber and minimally processed whole foods. These interventions address the root drivers of insulin resistance rather than manipulating individual macronutrients.
Bottom Line
Insulin and glucagon are not hormonal adversaries to optimize through extreme dietary manipulation; they are partners in a highly regulated system designed to maintain energy availability. Understanding how they work together demystifies a lot of the more sensational nutrition claims. Metabolic health is supported by the same lifestyle fundamentals that drive good health outcomes generally: consistent movement, quality sleep, and a sustainable, whole-food-based diet.